HIP REPLACEMENT
Thanks to close partnerships, surgeons and prosthesis manufacturers have made very significant progress concerning hip prosthesis during these last few years.
The quality of prosthesis materials has been enhanced, surgery technics have been fine-tuned, and robotics mixed with advanced software have been certified for surgery utilization.
Hence, the TKA surgery is now much less risky and is very likely to benefit to patient.
The quality of prosthesis materials has been enhanced, surgery technics have been fine-tuned, and robotics mixed with advanced software have been certified for surgery utilization.
Hence, the TKA surgery is now much less risky and is very likely to benefit to patient.
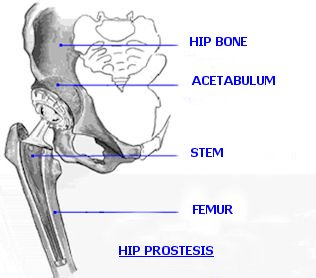
HIP PROSTHESIS COMPONENTS
When you get a TKA surgery, all parts of your hip joint are replaced by artificial components.
These components must be perfectly adapted to each patient in terms of size, geometry, form factor, structural materials as well as coated materials. The surgery technic is also specific to each patient.
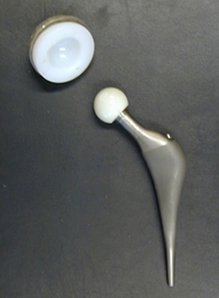
Generally speaking, a hip prosthesis consists in 2 main parts: the first one is a stem that goes into the femoral bone, the second one is a metal shell with a plastic joint, going into your hip (acetabular part).
These components can be cemented or not, depending on the prosthesis type.
These components must be perfectly adapted to each patient in terms of size, geometry, form factor, structural materials as well as coated materials. The surgery technic is also specific to each patient.
Generally speaking, a hip prosthesis consists in 2 main parts: the first one is a stem that goes into the femoral bone, the second one is a metal shell with a plastic joint, going into your hip (acetabular part).
These components can be cemented or not, depending on the prosthesis type.
TECHNICALS DETAILS
MINI-INVASIVE SURGERY
These surgery technique has been first implemented in the USA and has been escalated as an international method to cut the scar size by 50% as well as to preserve the soft tissues around the hip. This technique is now well recognized and an international course exists for surgeons who are willing to practice it.Beyond the scar size, this mini-invasive technique has multiple other benefits, such as bleeding reduction during the surgery, pain reduction after the surgery, a faster recovery and a reduction of the hospital stay. I have been using this mini invasive technique since 2005. This technique can be implemented to a broad majority of patients.
COMPUTER AIDED SUGERY
I started to use the computer aided surgery (CAS) techniques in 1999 when robotics started to be utilized in surgery rooms. From then, I improved my knowledge and my practice of computer in orthopedic surgery thanks to my membership of the International Society for Computer Assisted Orthopaedic Surgery. This membership provides me with a solid knowledge, fruitful exchange and discussion as well as state-of-the-art documentation on computer utilization for the surgery domain.Computer enables us to very accurately navigate all along the surgery process and to perfectly place each component of the prosthesis.
ENHANCED RECOVERY AFTER SURGERY
This specific process was deployed in France in 2014. It enables to drastically reduce the length of the hospital stays to a couple of days up to few hours. In this case, you are likely to get back home by your own the same day of the surgery. This technic is a real breakthrough within the patient care pathways. The ERAS technique is very beneficial to the medical team and the patient. As such, I decided to allocate an entire paragraph of my website to explain this ERAS process. You can have detailed information by clicking here : ERAS.Since I’m extensively practicing the ERAS method, I’m promoting this method to doctors during lectures and keynote talks in conferences and university courses. I also welcome and train other surgeons who would like to better know the ERAS process.
AMBULATORY PROSTHETIC SURGERY
I started to use the ambulatory process for hip and knee prosthesis in the summer of 2016. Since then, I adopted this process on a regular basis. Ambulatory process enables the patient to return home the same day. Initially implemented in the USA, this process is now proposed to 2 out of 3 patients for the hip prosthesis, and one out of 2 patients for the knee prosthesis.Some private hospitals are fully dedicated to ambulatory process such as the Monticelli-velodrome private hospital that started its operation in November 2016. To learn more click here.
WHAT ARE THE BENEFITS OF A TOTAL HIP ARTHROPLASTY
When your recovery period will be over, you will realize how awesome your benefits are :
Despite these benefits, surgeons usually recommend avoiding some sports such as running or jumping and any other sports that create strong shocks. But most of patients will be able to practice tons of sports such as walking, dancing, biking, horse riding, skiing and skating, swimming, golf, …
- Drastic pain reduction up to total pain removal
- Enhanced mobility, recover full movements
- Legs length adjustment
- Stronger legs
- Enhanced quality of life
Despite these benefits, surgeons usually recommend avoiding some sports such as running or jumping and any other sports that create strong shocks. But most of patients will be able to practice tons of sports such as walking, dancing, biking, horse riding, skiing and skating, swimming, golf, …
WHAT ARE THE RISKS OF A TOTAL HIP ARTHROPLASTY
Any surgery will come with a certain level of risk. You have to clearly understand those risks before your surgery and your surgeon will explain you what they are.
Dislocation : it happens only for 1% of patients. Most of the time, dislocation occurs during the first month after the surgery. If it happens, your surgeon will have to reduce the dislocation of your hip and you will get a full anesthetic process.
Infection : this risk is also pretty low, roughly 1%. The infection due to bacteria, can come from the environment or from the patient. You will have to be very cautious with your personal hygiene all along your recovery period and later. In fact, any infection occurring in your body (dental, urinary, lungs, …) could contaminate your hip prosthesis.
Phlebitis - Pulmonary embolism : in order to prevent any blood clot, your surgeon will prescribe you anti-coagulant drugs after your surgery. All your medical team, including your physiotherapist, will ask you to walk as soon as possible after your surgery: walking is the best way to avoid blood clot issues.
Hematoma : it is a normal situation to get a hematoma after a THA. If this hematoma becomes too large, it will put pressure on your hip tissues and that could be an issue. You will have to organize a visit to your surgeon who will take appropriate actions.
Other complications can occur after your surgery such as :
Dislocation : it happens only for 1% of patients. Most of the time, dislocation occurs during the first month after the surgery. If it happens, your surgeon will have to reduce the dislocation of your hip and you will get a full anesthetic process.
Infection : this risk is also pretty low, roughly 1%. The infection due to bacteria, can come from the environment or from the patient. You will have to be very cautious with your personal hygiene all along your recovery period and later. In fact, any infection occurring in your body (dental, urinary, lungs, …) could contaminate your hip prosthesis.
Phlebitis - Pulmonary embolism : in order to prevent any blood clot, your surgeon will prescribe you anti-coagulant drugs after your surgery. All your medical team, including your physiotherapist, will ask you to walk as soon as possible after your surgery: walking is the best way to avoid blood clot issues.
Hematoma : it is a normal situation to get a hematoma after a THA. If this hematoma becomes too large, it will put pressure on your hip tissues and that could be an issue. You will have to organize a visit to your surgeon who will take appropriate actions.
Other complications can occur after your surgery such as :
- Complication occurring during the surgery itself due to anesthetic or surgery acts, or due to prosthetic failure
- Neural or vascular post-surgery damage
- Functional complications related to non-compliance with postoperative instructions (immobilization time, rehabilitation modality ...)
- Complication due to other body parts such as the digestive system, the cardio-vascular system, the lung system,…)
HOW LONG WILL MY RECOVERY BE ?
Most of the time, your surgery will take place within the ambulatory unit of the hospital. Hence, you will be able to return home the same day. Sometimes, the patient stays at the hospital for the night and returns home the day after the surgery.
Your active recovery period will take place at your physiotherapist's office and will last for one month or so.
Very soon, you will walk without any walking stick and without any limp.
You will be able to practice gentle sports during your recovery period.
Depending on which type of job you do, you will be able to get back to work one month after your surgery date. If your job is physically intensive, you will have to wait 2 or 3 months before working again.
We will see each other to control the evolution of your recovery and of your prosthesis. I usually organize a check-up visit during the first month, one year after and then every 2 years. These visits are complemented with a clinical and x-rays controls.
Your active recovery period will take place at your physiotherapist's office and will last for one month or so.
Very soon, you will walk without any walking stick and without any limp.
You will be able to practice gentle sports during your recovery period.
Depending on which type of job you do, you will be able to get back to work one month after your surgery date. If your job is physically intensive, you will have to wait 2 or 3 months before working again.
We will see each other to control the evolution of your recovery and of your prosthesis. I usually organize a check-up visit during the first month, one year after and then every 2 years. These visits are complemented with a clinical and x-rays controls.
FAST RECOVERY FOR HIP REPLACEMENT
This recovery process is dedicated to hip prosthesis only. It works when the hip surgery has implemented the mini-invasive technic that preserve the soft tissues of the hip and also implemented the specific surgery process adapted for the Enhance Recovery After Surgery (ERAS) method.
This specific protocol has been designed with the partnership of Benjamin Thomas, physiotherapist at Frioul center.
As soon as the surgery day (4 to 6 hours after the surgery), you will stand up from your bed for the first time with the help of the physiotherapist. The goal is to make your home return possible the same day.
This will be possible if all the physio criteria are checked. These criteria can be reached very early after your surgery and then you can go back home.
Therefore, It is mandatory that you come to the hospital with your walking sticks and with appropriate shoes (with laces). At this step, you won’t have any drains and as such you will be able to wear loose clothing. You will have dinner with a normal manner : that is at the table, not in your bed. Bear in mind : you are not sick, you've just had surgery !
Your fast return to your home is key for your recovery. All your surgery process will be implemented to simplify the post-surgery procedure and allow a fast hospital exit: this will reduce the risks of surgery complications.
3 criteria :
This specific protocol has been designed with the partnership of Benjamin Thomas, physiotherapist at Frioul center.
As soon as the surgery day (4 to 6 hours after the surgery), you will stand up from your bed for the first time with the help of the physiotherapist. The goal is to make your home return possible the same day.
This will be possible if all the physio criteria are checked. These criteria can be reached very early after your surgery and then you can go back home.
Therefore, It is mandatory that you come to the hospital with your walking sticks and with appropriate shoes (with laces). At this step, you won’t have any drains and as such you will be able to wear loose clothing. You will have dinner with a normal manner : that is at the table, not in your bed. Bear in mind : you are not sick, you've just had surgery !
Your fast return to your home is key for your recovery. All your surgery process will be implemented to simplify the post-surgery procedure and allow a fast hospital exit: this will reduce the risks of surgery complications.
PHASE 1 (the day of your surgery)
You will go back to your hospital room without any drain nor splint. 3 criteria have to be checked to allow you an early exit from the hospital :3 criteria :
- An autonomous transfer from the prone position to the standing up position and back to the bed position
- Being able to walk alone and along the corridor, controlled by your physiotherapist, with or without sticks
- Going upstairs and downstairs
PHASE 2 (taking place at your physiotherapist office)
- Passive activation of your hip with a flexion/extension movement controlled by your physiotherapist
- Assisted active movement of your hip with flexion/extension in the prone position. Self-recovery training
- Transfer exercise: from prone position to standing up position and back to prone position.
- Walking alone with 2, then one and then without any sticks
- Going upstairs and downstairs
- Advices